6287 S. Redwood Rd #101 Taylorsville, UT
Call Us Today!
WE TRIED TO FIND THE BEST MOUTH GUARD FOR TEETH GRINDING

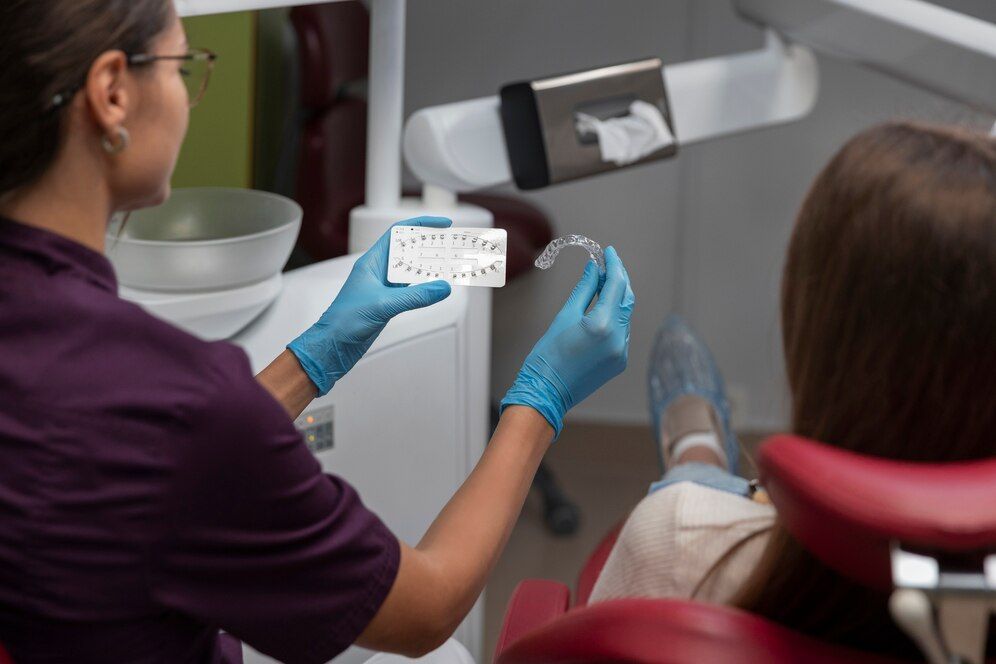
BEST MOUTH GUARD FOR TEETH GRINDING
Article originally published in The New York Times Wirecutter by journalist and author, Nancy Redd.
If your jaw or neck feels sore after you wake up, you may be one of the millions of people suffering from sleep bruxism—when a person involuntarily clenches their jaw and grinds their teeth at night or during a nap. Though estimates differ, typically 10% to 16% of adults regularly suffer from sleep bruxism. But this has been no typical year: Pandemic-related stressors are associated with an uptick in not just tooth grinding and jaw clenching but also cracked teeth and other bruxism-associated dental problems.
Unfortunately, mouth guards—which provide a small barrier between the teeth and are thought to protect against the effects of teeth grinding and jaw clenching—may not work. And they might even make things worse.
Readers have long asked us for recommendations of over-the-counter mouth guards for teeth grinding, as these are widely available and typically cost significantly less than mouth guards fitted by a professional (with or without dental or medical insurance coverage factored in). For weeks, we molded and used seven boil-and-bite (those you soften with hot water and then bite into for a “custom” fit) and four ready-to-wear nighttime mouth guards in an attempt to find the best options for most people. We then identified the over-the-counter mouth guards we like best. However, after speaking at length with multiple dentists, sleep specialists, and bruxism researchers, we learned that, in most cases, wearing a mouth guard is not enough to treat bruxism, and in some cases, it can actually cause additional harm, as our New York Times colleagues have reported on, as well.
"There’s a misconception about mouth guards that they prevent people from tooth grinding,” said Dr. Jamison Spencer of The Center for Sleep Apnea & TMJ in [Salt Lake City, Utah and] Boise, Idaho, who in the past has received samples from a company that makes bruxism treatment aids. Instead, mouth guards “provide teeth something to grind on other than other teeth,” he said. “Alone, they solve no dental problems.”
At best, an over-the-counter mouth guard can serve as a stopgap solution to prevent further tooth damage while the wearer awaits professional dental or medical care to try to figure out the root causes of their bruxism. But at worst, an over-the-counter mouth guard can make underlying conditions (aging dental work, gum disease, or inflammation) worse “and require more invasive and traumatic treatment once the person finally goes to the dentist,” said Dr. Leena Palomo of the Case Western Reserve University School of Dental Medicine.
See a professional first
Spencer referenced studies showing that tooth grinding and jaw clenching in some people who suffer from untreated sleep apnea worsened with mouth guard use. Furthermore, “drugstore mouth guards,” as Dr. Samantha Rawdin, a prosthodontist who treats complicated dental and facial problems at Gallery57 Dental in New York City, calls them, “are made from softer, squishier plastic [compared with medical-grade guards] that can make some people clench their teeth more, defeating the purpose.”
Alan G. Glaros, a professor emeritus at the University of Missouri–Kansas City, agreed: “They’re usually spongy and soft, so people tend to chew them up quickly, and they kinda gnaw on them in addition to their regular grinding.”
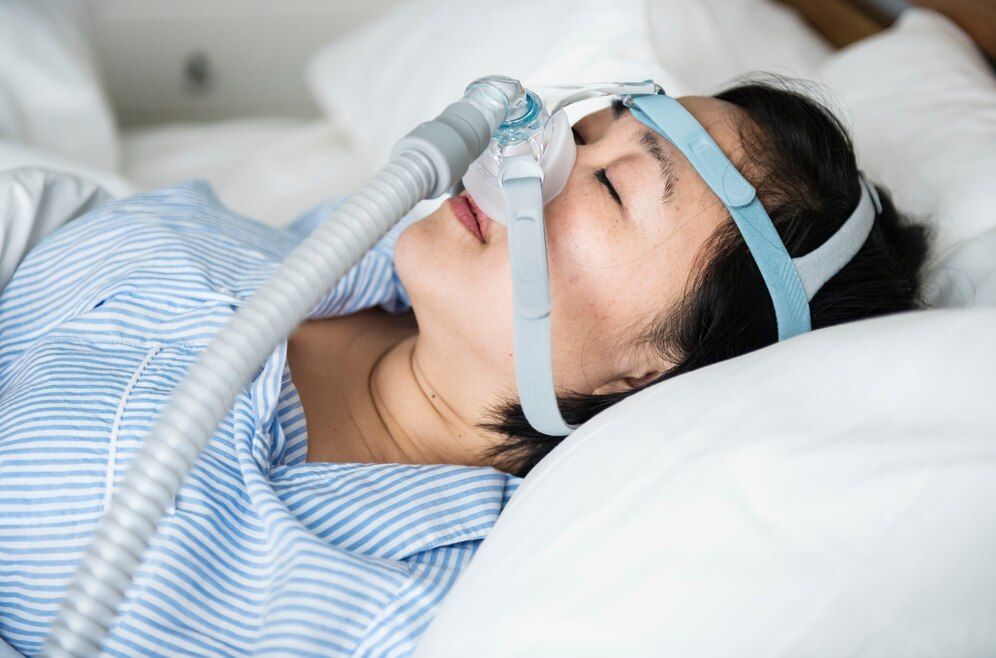
Yet a dental or doctor visit for a custom (and likely, hundreds of dollars more expensive) mouth guard isn’t always the answer, either. “If a patient just goes to the dentist and gets a mouth guard without receiving any additional information about how to improve or control the bruxism,” said Spencer, “it’s like buying a helmet to wear because you’ve been banging your head against the wall for years, without finding out why you’re still banging your head.” Similarly, Rawdin encourages grinders to specifically seek an oral-health professional with expertise in treating the causes of bruxism to “properly examine and diagnose what detrimental habits have formed, and thus what the best treatment is to meet needs,” which can extend well beyond the use of mouth guards. Botox injections, for example, are an alternative treatment Rawdin has used to treat patients with bruxism. Other treatments include dental appliances such as bite plates, CPAP machines for sleep apnea, and physical therapy including jaw, neck, and head massage or exercises. Also, any activities that reduce stress, such as meditation or exercise, can help. “When stress levels decrease, so do habits induced by stress, like bruxism,” said Rawdin.
Identify the causes of bruxism
Realizing that mouth guards were not the panacea to nighttime teeth grinding we had hoped for, we sought alternatives to recommend, only to come up relatively empty-handed. “I’ve been researching bruxism for over 40 years, and you’d think after all this effort and time we’d be further along in terms of identifying successful treatments, but we aren’t,” said Glaros. “What we have learned since my very first paper on the topic in 1977 is that bruxism is not a dental disorder, nor is it a sleep-related disorder, but it must be seen, and studied, as both, which complicates the researching process.” Since there is no good animal model available for researching bruxism, studies have to be done with humans, which is “slow, hard, and very expensive work,” Glaros said. That makes it difficult for researchers to develop pharmacological treatments or other approaches that could help sufferers. “It’s very frustrating because it’s such a common issue, and there’s no good way to treat it.”
“Sometimes you can’t stop the stress or solve the core issues, so you have to play defense,” noted Rawdin. “If you can’t turn off the grinding, you want to get a properly fitted and frequently adjusted mouth guard to grind on to save your teeth.”
Glaros, too, warns against using over-the-counter mouth guards without consulting a professional, or over the long term. But he considers them potentially useful for protecting teeth in the short term: Just as you apply a bandage to protect skin, “you can use a mouth guard to protect your teeth” temporarily.
If you can’t afford or access a proper oral exam to diagnose and treat the cause of your bruxism, all of our experts suggest searching for a nearby dental school or federally qualified health center (FQHC) that has a dental service attached, as these institutions usually offer treatment for less. “Access to care is a challenge,” acknowledged Palomo, “but calling around different places, explaining your circumstances, and asking for pricing and payment plans can work, as different practices and clinics offer different options.”
Consider an OTC mouth guard for temporary use
If you’re simply attempting to protect your teeth until you can get to a dentist, of the 11 over-the counter nighttime mouth guards we tested, we found two boil-and-bite models to be the most comfortable and easy to use. Our favorite overall, the Neomen Professional Dental Guard, is available only online but is one of the slimmest and easiest-to-mold guards we tried (using hot water and a strong bite), as well as one of the least expensive at $20 for a pack of four. The thicker Dentek Professional-Fit Dental Guard, which at $25 for one is more expensive than the Neomen, is readily available in drugstores and nearly as simple to mold. Both come with hardshell cases peppered with small air holes to keep the guards clean and dry, and both are easy to clean (with a toothbrush and toothpaste). As for an ultra-slim, ready-to-use option (no boiling required), disposable Plackers Grind No More Dental Guards (about $20 for a pack of 16) may help shield your teeth from the worst effects of grinding until you can see a pro. Our testers found these easier to tolerate than the bulkier mouth guards we recommend.
However, even if an over-the-counter mouth guard seems to “work,” remember that “they aren’t treating the actual issue, and regular visits to the dentist are very important, even during the pandemic,” said Palomo. “It is not normal or healthy to have tooth pain or a jaw that clicks or hurts, and ignoring, denying, or covering it up will not make it go away.”
Sources
- Alan G. Glaros, PhD, professor emeritus, University of Missouri–Kansas City, phone interview, February 9, 2021
- Jamison R. Spencer, DMD, MS, The Center for Sleep Apnea and TMJ in Salt Lake City, Utah and Boise, Idaho, phone interview, February 8, 2021
- Samantha B. Rawdin, DMD, prosthodontist and owner of Gallery57 Dental, phone interview, February 8, 2021